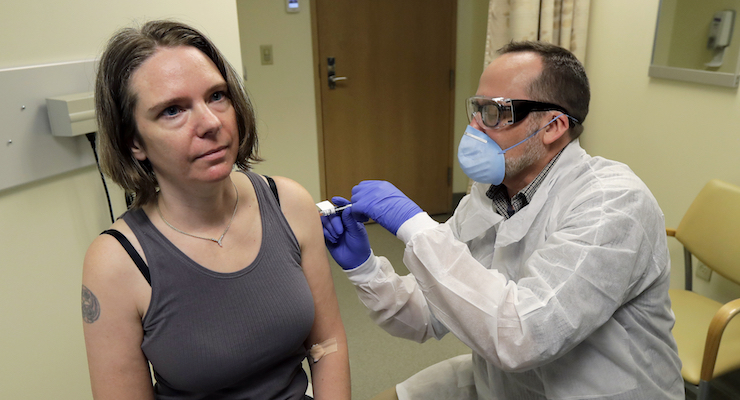
Several COVID-19 vaccines are in the final stages of testing, with pharmaceutical companies Pfizer and BioNTech announcing Monday their vaccine is effective in preventing the virus in 90% of participants.
While it’s great news, widespread distribution of the vaccine is still a while away, and most Australians will have to wait until late next year to get the shot.
Here’s what needs to happen before then.
Step one: full analysis
Exciting as Pfizer’s interim announcement is, the trial still needs to run its course, Sydney University lecturer in bioethics Dr Diego Silva told Crikey. Trials have been sped up, with results released from the final phase in months instead of years.
Next, journals will pick up Pfizer’s report and send it out for peer review.
“Peer review is the way we verify that there’s credibility in the science itself. It’s a very rigorous process,” he said. This could take a few weeks.
The data would then be made public for other scientists to scrutinize.
Step two: commit to buy
Next, Australia’s Therapeutic Goods Administration (TGA) would get involved, analysing results to see if the vaccine should be approved in Australia and purchased by the government.
“The TGA considers all the evidence … and makes a decision not just on whether it should be made available but also on what — and who — it’s being used,” University of Queensland infectious diseases epidemiologist Linda Selvey told Crikey.
Australia already has deals to buy vaccines from five pharmaceutical companies, as long as the TGA deems their vaccines to be safe and effective. Some vaccine candidates have been allowed to pre-apply for TGA registration to speed up the approval process.
The vaccines would then be added to the Pharmaceutical Benefits Scheme, making them free for the public.
Step three: manufacturing ramps up
Generally, manufacturing doesn’t start until the vaccine is given the green light by governments. But because billions of doses are needed to beat this pandemic, manufacturing has already begun for a number of vaccines.
Australia has facilities to manufacture protein-based vaccines. We’re already producing AstraZeneca and the University of Queensland’s vaccine. Manufacturing enough for the country could take up to 12 months.
We don’t have onshore facilities to manufacture mRNA vaccines, like Pzifer’s, and would have to ship doses in. Pzifer has also started manufacturing, hoping to make 100 million doses this year and 1.3 billion in 2021.
Step four: storage solutions sorted
Where we store millions of doses of the vaccine is another issue. While all vaccines need to stay cold, mRNA vaccines need to be in stored in freezers at -70 degrees.
“We’d have [the freezers] on hand in most large hospitals and labs, but not widely available across all of Australia,” Selvey said.
Many vaccines also require two shots, doubling efforts.
Step five: priority groups vaccinated
Identifying who should get the vaccine first isn’t as easy as it sounds, Silva says.
“There are a lot of discussions that priority should be given to vulnerable groups, and it may very well be the case, but it will depend on the actual science itself,” he said.
Trials will show who the vaccine is most effective on, and these people might be prioritised ahead of the vulnerable.
While it’s likely Australia will start vaccinating vulnerable groups and frontline workers, young individuals who are more likely to be vectors for the virus could also be prioritised.
“The devil is in the details and it really matters that we have those to make our decisions ethically defensible,” Silva said.
To be effective, 60-70% of the population needs to be vaccinated.
La Trobe University infectious disease epidemiologist Dr Hassan Vally told Crikey many of these steps were occurring at the same time because of the sheer scale of the pandemic.
“We’re doing parallel processing,” he said. “The plan is to shave off a whole lot of time taken to develop the vaccine and in the manufacturing process.”
We’re also likely to have more than one vaccine available in Australia.
Step six: watch, wait and tweak
Because the vaccine is so new, and long-term studies haven’t been completed, scientists would keep monitoring the effect of the vaccines and tweak them as needed. We still don’t know if any vaccine has a long-term effect.
“It may turn out the vaccines have different characteristics and properties,” Vally said. There’s also the possibility combining vaccines produces a stronger response, known as prime boosting.
“Some may provide stronger immunity or require one dose instead of two,” he said.
An annual booster of the vaccine, similar to the flu shot, may also be necessary to deal with virus mutations.







I work in the U.A.E. for the Abu Dhabi Health Services Company which manages the public health services across Abu Dhabi. The Sinopharm vaccine has passed stage 3 trials here, been found safe and effective, and is being rolled out to both frontline and support staff in the healthcare sector. I received my first shot three weeks ago and will get my booster shot tomorrow.
I’m returning to Australia in a couple of weeks and while I wholeheartedly agree with the current quarantine approach, it will need to evolve as more Australians return who have already been vaccinated. I might be among the first but I won’t be the last! Perhaps that evolution would see a reduction in the number of quarantine days required for vaccinated returned travellers, which would free up spaces for more Australians to return home. It won’t happen for me, but I don’t get the sense there is any policy thought or development happening in this space.
Regards,
Simon
Please keep us posted on your progress, it’d be nice to read something without a blatant ulterior motive.
Will do. I believe the outcome of the Sinopharm trial here will be published next week.
Adding a vaccine to the PBS does not make it free to the public. A copayment is required, apart from healthcare/pensioners who have already reached their contribution limit for the year.
Normally free vaccines are available and administered via GPs or pharmacies and funded by State governments. Even though funded federally, this established distribution modality will probably be used.
Since two injections – three weeks apart – are likely to be required, careful recording and recall systems will need to be in place to ensure that essential second dose is given.
It is entirely a political decision, it doesn’t have to be part of the PBS. If govt wants a high percentage of coverage it will likely be given out for free. There is nothing in legislation or PBS preventing them from making policy decisions as they see fit.
The prioritisation issue is more a sociological and philosophical issue than a pure ‘science’ issue. Do you aim to stop the spread or focus on mitigating immediate impact?
Delays and shortages but no mention of the dreaded compulsory vaccinations!
It’s a plot to lull us into complacency!
Or is it just being hidden until the 5G tower network is complete?
B—o
They are not ready yet. It has to be combined with major world-wide catastrophic events.
There has already been a contract awarded for the construction of one on the Moon which will blanket the Earth with Death… oops, Mind Control rays –
https://edition.cnn.com/2020/10/18/tech/4g-network-moon-trnd/index.html
Travel and other rights will be restricted to people who are vaccinated. So it would be good to have a digital International Certificate of Vaccination or Prophylaxis (ICVP) or carte jaune or yellow card.
The International Immunisation Certificate was the norm until the 70s – arguably more important a travel document than a passport.
There were a lot of painful arms at the start of Kangaroo Route back in the day.
I cannot see how such jacked-up travellers will not soon again be de rigeur.